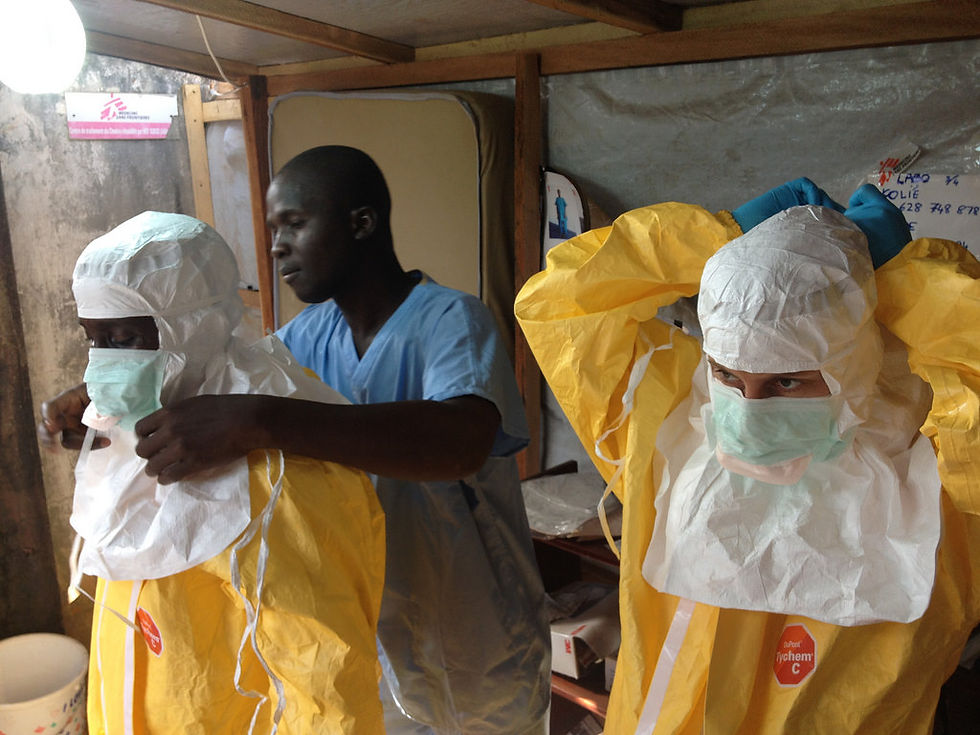
Ebola Yesterday
History would make us believe that Ebola is a deadly disease that is unique to Africa; however, unless you’ve lived on the continent, you might be unaware of the true impact this virus has on the African community. The Ebola virus (EVD) is a recurring zoonotic illness that is located mainly in sub-saharan Africa (World Health Organization, 2022). EVD is rare, but it is a severe illness that can be fatal in humans. Making its introduction in the Democratic Republic of Congo in 1976 with a mortality rate of 88%, it became evident that this virus was capable of eradicating entire communities (CDC NCEZID, DHCPP, VSPB, 2021). At first, public health officials presumed that these outbreaks were from an isolated event hosted by a person who traveled abroad, but soon discovered that the early attacks of EVD were caused by two genetically distinct viruses (CDC NCEZID, DHCPP, VSPB, 2021).
Ebola Today
Almost 50 years later, there are still outbreaks occurring in its country of origin and is starting to impact other countries due to increased international travel. One of the most significant Ebola outbreaks occurred fairly recently from 2014 until 2016, infecting over 32,000 West African people and killing 13,600 people (Bebell et al., 2017). During that time, what was once a disease that was secluded to African began to spread to first-world countries like the U.S., infecting 11 people and causing the death of two others. Seeing how bad the outbreak of 1976 was, and the impact of the millennial outbeak, why haven’t precautions been established to prevent a ramage of this highly infectious and fatal disease? It is understood that the case fatality rate, or the proportion of people diagnosed with EDV who end up dying of it, ranges from 25% to 90%, with an average case fatality rate of 50% (Patel & Shah, 2022). For comparison, the case fatality rate for COVID-19 was highest at 5.5% in Syria, excluding Korea as an outlier where six were diagnosed and one died (Johns Hopkins University and Medicine, 2022). Both diseases were easily transmitted, but death from COVID-19 was nowhere near as likely as it was for EDV. However deadly, the amount of research, time, and money put into finding out how to “stop the spread” of EDV from the U.S. from 2014-2016 was about $2.4 billion compared to $4.6 trillion - yes, trillion - on COVID-19 response (USA Spending, 2022).
Ebola Tomorrow
There was no treatment for Ebola until recently; if a person was infected previously, they were just told to monitor symptoms with supportive care. In a world where technology is evolving faster than ever, COVID-19 showed us that we have the capacity to roll out a new vaccine for an illness that was only a year old. That said, why is “supportive care” the initial medical response to a condition historically known for killing, on average, half those infected? Out of all six of the species within the Ebolavirus genus, two treatments were created for just one. Approved by the U.S. Food and Drug Administration two years ago, both Inmazeb and Ebanga were approved to treat only EVD caused by the Ebola virus species Zaire ebolavirus (CDC NCEZID, DHCPP, VSPB, 2021). It was deemed after the 2018-2020 Ebola outbreak that the survival rate was higher for those receiving treatment, but even with this, the same efficacy of the drugs has not been evaluated (CDC NCEZID, DHCPP, VSPB, 2021).
Ebola Forever
A challenging epidemic can have a devastating global impact on healthcare, the economy, and society. Our job as public health professionals is to ensure that we support our community, but one must ask the question, as in a previous post, how many more minorities must succumb to preventable diseases before American public health efforts target their safety? Suppose EVD spreads to other areas, like COVID-19 and Monkeypox, what is our game plan as a nation? Are we prepared for another outbreak, especially from a disease with a higher fatality rate than any other outbreak we have seen? Not only should we educate ourselves on ways to stop recurring outbreaks from transpiring, but we also need to support these areas where outbreaks are more common - as that may not always be the case. We need to be proactive, and not reactive; the former is our answer on how to “stop the spread.” We use contact tracing to pinpoint where a disease originated, but case investigations with such a fatal disease rate are not the best means of stopping the spread. As a country, we are continually given the answers to the test but are continuing to fail because we are not taking proactive measures to end preventable diseases before more people are killed.
Closing Remarks
Ebola is just one of many diseases that we do not speak about until it becomes an issue where the rich (e.g., white Americans) are affected. For instance, did you know that there were outbreaks in two cities of the Democratic Republic of Congo and one Ugandan city THIS YEAR? We have seen this story more often now and the main question is, when will we write the happy ending to it? It is exhausting and offensive to the field that we are not made aware of diseases that have been around for half a century, but can make a vaccine to help but a small portion of the world. A woman traveling back from her village in Africa stated that we [Americans] are not even aware of the impact Ebola has on someone who has the disease. Why is it that we are so far removed from something that can wipe out a community but are able to fund a disease that has become a condition that we can live with in “normality” such as COVID-19? If we do not start being proactive instead of reactive, we will not have the opportunity to “stop the spread,” rather, we will be forced to live in another lockdown (or worse) to ensure that the case fatality rate does not wipe out our country and beyond.

Commentaires